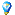source:
https://www.tandfonline.com/doi/full/10.1080/03036758.2011.557036#:~:text=Since%20the%20mid%2D1990s%20the,criminalise%20the%20substance%20in%202008.
When I last went to NZ for a skiing holiday, NZ had legislated to legalise Class D drugs (social tonics) and you could buy
piperazinesWiki for around $NZD 15 each. I bought some
TFMPPWiki and
BZPWiki for $NZD 20 but I did not enjoy them. The were supposed to mimic amphetamine and MDMA respectively.
This is the story of legal piperazines in NZ's bold experiment.
Benzylpiperazine in New Zealand: brief history and current implications16 Mar 2011
AbstractOver the last decade, New Zealand has led the world in the legal sale and uncontrolled use of the recreational drug benzylpiperazine (BZP), the active ingredient of ‘party pills’. One survey found that 40% of 18–29-year-olds admitted to using BZP-based party pills while, in another study, 44% of first-year university students had used the drug. During the period it was legally available for sale, BZP usage in New Zealand far exceeded the usage of any illicit drugs other than cannabis.
In 2005 the New Zealand government created legislation intended to regulate the drug, but as potential health risks from BZP consumption became apparent, subsequent legislation was introduced to prohibit the substance. In 2008, the sale and possession of BZP was criminalized, with the result that (a) some users possibly switched to other illegal drugs, and (b) a market developed for alternative party pills that are BZP-free but contain unregulated substances that may themselves pose a health risk.
The following review briefly covers the scientific and legal background of benzylpiperazine with particular reference to New Zealand, the country in which it was most popular.
IntroductionBenzylpiperazine (BZP; Fig. 1) is a drug that produces amphetamine-like effects in humans, including an elevated sense of energy and euphoria. Since the mid-1990s the chemical has been reported to have been used as a recreational stimulant. From 1999 onwards, the drug was legally marketed in New Zealand. The chemical gained widespread popularity among New Zealand youth as a legal party drug until the government moved to criminalise the substance in 2008. This review briefly covers the history and pharmacology of BZP before exploring clinical and sociological research pertaining to the compound's use as a recreational stimulant in New Zealand. The drug's changing legal status is summarized and the repercussions of criminalising BZP sale and possession are discussed with reference to other legal and illegal psychoactive substances.
Fig. 1 Chemical structure of benzylpiperazine.References
 Development of BZP
Development of BZPBenzylpiperazine is a compound belonging to the class of chemicals called piperazines. It was originally synthesized by researchers from Burroughs, Wellcome & Co. (Baltzly et al. Citation1944). It is widely stated that the chemical was synthesized for experimentation as a de-worming agent for cattle but research was abandoned in favour of more promising piperazine compounds (for example see McNamara [Citation2009]; originally stated in Campbell et al. [Citation1973]). However, there is no published research pertaining to the use of BZP as treatment for intestinal parasites, and the synthesis of BZP is believed to pre-date Burroughs, Wellcome & Co.'s interest in piperazines as anti-helminthics. Although the files relating to the development of BZP appear to have been lost, it has been stated by a Wellcome employee (AW Peck) that BZP was originally developed as a potential anti-depressant (EMCDDA Citation2005). Following the Baltzly et al. (Citation1944) synthesis,there was little further investigation of BZP in the literature until human studies were performed in the early 1970s, exploring the drug's suitability as an anti-depressant (see ‘Early research on BZP’ below). A speculative patent for BZP-derived antidepressants was filed by Wellcome researchers in the 1960s (Barrett et al. Citation1968), and stated that BZP was effective in reversing various pharmacological animal models of depression. No such application of BZP ever eventuated.
Pharmacological properties of BZPIn vitro and animal studies have shown that BZP causes an increase in the release of the monoamine neurotransmitters noradrenaline, dopamine and, to a lesser extent, serotonin in the rat central nervous system (Tekes et al. Citation1987; Baumann et al. Citation2005) and synaptosomal preparations (Rothman & Baumann Citation2006). The exact mechanism by which BZP causes the increase in neurotransmitter release has not been elucidated, although there is evidence that BZP may block the dopamine transporter complex DAT, preventing neurons from removing released dopamine from synapses (Baumann et al. Citation2005). Benzylpiperazine has also been shown to inhibit the reuptake of monoamine transmitters in synaptosomal preparations (Nagai et al. Citation2007) and has no impact on G-protein activity in cortical membranes, indicating a lack of metabotropic action (Nonaka et al. Citation2007). When BZP is combined with 3-trifluoromethylphenylpiperazine (TFMPP; a serotonin-mimicking piperazine often included in commercial BZP ‘party pills’) the increased release of dopamine and serotonin is very similar to that produced by MDMA (3,4-methylenedioxymethamphetamine,the definitive ingredient in recreational ‘ecstasy’ pills sold on the black market; Baumann et al., Citation2005).
In agreement with such observations, animal behavioural studies indicate that the effects of BZP are rewarding. Rats display conditioned place-preference when given BZP, repeatedly returning to the location in which the drug was administered (Meririnne et al. Citation2006). Primates given free access to intravenous BZP will repeatedly self-administer the drug when given the opportunity (Fantegrossi et al. Citation2005). Both of these phenomena are typical of other drugs of abuse such as heroin, cocaine and methamphetamine (Bardo & Bevins Citation2000; Freeman et al. Citation2010).
The absorption and excretion profile of BZP has been examined in humans by Antia et al. (Citation2009), who found that after a 200 mg oral dose of BZP, plasma concentration peaks 75 min after dosing, with a half-life of 5.5 h. Analysis of urine revealed that in addition to BZP, hydroxlated BZP (4-OH BZP and 3-OH BZP) and trace amounts of sulfate-conjugated metabolites (N-sulfate BZP and O-sulfate BZP) could be detected. Liver enzymes CYP2D6, CYP1A2 and CYP34A have been shown to metabolize BZP. In vitro studies show that BZP interferes with the metabolism of other substrates for these enzymes, suggesting a potential for drug–drug interactions (Murphy et al. Citation2009; see Antia [Citation2009] for a comprehensive review of BZP pharmacokinetics and metabolism).
Early research on BZPThe effects of BZP on humans were first published in 1973. Wellcome Research Laboratories conducted two double-blind studies in which drug-naive participants (Bye et al. Citation1973) and former amphetamine addicts (Campbell et al. Citation1973) were given oral doses of either BZP or dexamphetamine. Participants were subjected to a series of tests to determine the similarity of the little-studied BZP to the better-characterised dexamphetamine. Both studies found that the objective and subjective (questionnaire-based) effects of BZP were very similar to dexamphetamine. In light of the subjective responses from the addicts in the Campbell et al. (Citation1973) study, the authors concluded that BZP was a potential drug of abuse. The addicts noted the stimulating and pleasurable effects of the drug and responded positively to questions such as ‘would you like to take the drug every day?’ The authors closing statement advised that BZP, which was freely available from chemical suppliers, be placed under statutory control. This suggestion was ignored by US and European authorities and BZP remained legal and accessible. Until very recently these studies were the only published human experiments in which the effects of BZP were monitored in a controlled environment.
Despite the findings and warnings of the Wellcome researchers, a Hungarian company, EGIS research, trialled a BZP-derived compound in humans as an antidepressant during the 1980s. The drug, Trelibet (EGYT-475; N-benzyl-piperazine-piconyl fumarate), was found to be metabolised to active BZP in humans. There is evidence that Trelibet reached phase I and II clinical trials (Nogradi Citation1984; Magyar Citation1987); however, clinical studies in humans were apparently cut short due to undesirable amphetamine-like side effects (unpublished work discussed in Thompson et al., Citation2006). A further BZP pro-drug, befuraline (DIV-145; 1-benzofuran-2-yl(4-benzylpiperazin-1-yl)methanone), was trialled as an antidepressant during the same period. In the treatment of depressed patients, befuraline was shown to be as effective as imipramine, with limited side effects in phase II clinical trials (Gastpar et al. Citation1985; Conti et al. Citation1988). No further clinical research on befuraline has been undertaken. Although there is evidence that first-pass metabolism of befuraline produces active BZP (Johnson Citation1980; Conti et al. Citation1988), the drug has been largely overlooked in recent literature examining BZP.
BZP as a recreational drugIn 1996 the first recreational ‘underground’ use of BZP was recorded by the Drug Enforcement Agency (DEA) in California. Usage of the drug remained minimal for several years until the turn of the twenty-first century, at which point agencies and governments began to take notice of a growing trend in which they found the widely popular drug MDMA was occasionally mixed with BZP in tablets. In 1999 BZP was added to the European Union's ‘Early Warning System’ designed to monitor the patterns of use for new potential drugs of abuse (EMCDDA Citation2005).
Despite the concerns of authorities, recreational use of BZP remained very limited throughout the USA and Europe although isolated incidents of BZP possession were recorded. In most cases, BZP was assumed to be a cheaper substitute for MDMA in tablets intended to be sold as ‘ecstasy’ to unwitting customers (EMCDDA Citation2005). In the last decade BZP has also been used for its stimulant properties in the fields of horse racing (Barclay Citation2003) and athletics (Tutty Citation2005), where its use has now been explicitly prohibited (ARCI Citation2010; WADA Citation2010).
BZP use in New ZealandWhile Europe and the USA experienced little BZP use in the early 2000s, a legitimate market arose in New Zealand. Entrepreneur Matt Bowden is credited as the individual responsible for introducing BZP-containing party pills as a commercial product. Formerly addicted to methamphetamine, Bowden, with the aid of an unnamed neuropharmacologist,
identified BZP as a possible ‘low-risk’ substitute for methamphetamine. In 1999, Bowden started his New Zealand company Stargate International (
www.stargateinternational.org), which presented BZP-containing pills as a safer, legal alternative to illicit drugs. After corresponding with government agencies over the legality of the then uncontrolled substance, Bowden began to market BZP pills initially as a ‘harm minimisation tool’ to aid methamphetamine users in escaping their addictions (Bowden Citation2004; May Citation2006).
In the following years BZP became popular amongst youth in the dance/rave scene as a potent stimulant with euphoric properties and marketing of the drug expanded rapidly (Sheridan et al. Citation2007). As BZP consumption increased, the chemical was combined in pill formulation with TFMPP, another piperazine that in combination with BZP has been shown to produce effects similar to MDMA in mice (Baumann et al. Citation2005). The products were aggressively marketed as a ‘legal high’ and sported enticing brand names such as ‘Frenzy’ ‘Rapture’ and ‘Charge’. BZP dosages ranged from 70 to 500 mg across brands and were often combined with 10–25 mg of TFMPP (Thompson et al., 2006).
The Social Tonics Association of New Zealand (STANZ), a coalition of major party pill producers, attempted to self-regulate the industry by encouraging age limits, maximum dosage (200 mg per dose) and a code of practice (Wilkins & Sweetsur Citation2010). However, there was no official regulation of BZP until 2005 and, even then, the many potential regulations were not enforced (see ‘Legality of BZP in New Zealand’ below). Party pills could be sold anywhere, at any dose, to anyone. According to media sources less scrupulous retailers took advantage of the market opportunity created by STANZ guidelines to supply high-dose pills with no quality control (Martin Citation2004; McKenzie-McLean Citation2006). By 2008, industry sources estimated that 26 million pills had been sold in New Zealand (STANZ Citation2008).
Prevalence and adverse effects of BZP consumption in New ZealandAs recreational use of BZP became widespread, studies were conducted to examine the extent and ramifications of BZP consumption. Wilkins et al. (Citation2006) conducted a comprehensive survey of New Zealanders and found that in a sample of 2010 individuals aged 13–45, 20% had taken BZP at some point in their life, with 42% of these users having taken BZP in the last 12 months. Among the 18–29-year-old subgroup, prevalence of lifetime use doubled to 40%. The authors also noted 30% of users had on some occasion exceeded the recommended dosage. Another survey found that 44% of first-year university students had tried BZP (Bryson & Wilson Citation2007). These surveys also examined the prevalence of other drug use in the sample and showed that BZP use was much more common than the use of any illicit drug aside from cannabis.
Further survey data also revealed that 89% of BZP users combined the pills with other drugs, most commonly alcohol and tobacco. Adverse physical symptoms were often reported by BZP users, with insomnia (54%), headaches (26%) and nausea (21%) being the most commonly experienced (Wilkins et al. Citation2008). Despite indications from animal studies and early human studies, BZP does not appear to be physically addictive. The Wilkins et al. (Citation2006) survey found very little evidence of addiction amongst BZP users.
The more serious potential side effects of BZP use were first highlighted by Gee et al. (Citation2005) in a study of hospital admissions. All data from party-pill related admissions to a Christchurch emergency hospital ward were recorded and analysed. Amongst the 80 party pill-related admissions (which included instances where BZP had been consumed with other substances) in a 5-month period, palpitations, vomiting and agitation were the most common recorded side effects of BZP ingestion. Disturbingly, 15 toxic (i.e. non-epileptic) seizures were recorded among patients. The results of Gee et al. (Citation2005) contrast with a similar study from the Auckland Hospital Emergency Ward. Over a 3-year period (cf. 5 months in Gee et al., Citation2005), only 26 BZP-related admissions were recorded and no seizures reported (Theron et al. Citation2007). The discrepancy between these two emergency ward studies could be in part be explained by the availability of stronger-dosage brands of BZP pills in the South Island, where industry regulation of the quality and standard of BZP products was less stringent—although this is poorly supported by available survey data. It is also possible that differing local attitudes towards BZP led to Christchurch users mixing BZP with other illicit drugs more often (Wilkins & Sweetsur Citation2010). Thompson et al. (Citation2009) conducted the first modern controlled study of BZP (and the common co-ingredient in party pills, TFMPP). They found that in a sample of previous BZP users, two 150 mg doses of BZP/TFMPP over 2 hours alone or in combination with six standard units of alcohol caused serious side effects in some participants, including hallucinations, agitation and vomiting. The severity of the side effects led the researchers to discontinue the study halfway through due to ethical concerns. The study also investigated the effects of BZP/TFMPP pills on the participants’ driving abilities using a simulator. The researchers found that the pills significantly improved driving ability against baseline (in contrast to alcohol, which decreased driving performance).
A recent controlled study has revealed more information about the subjective effects of BZP in humans. Lin et al. (Citation2009) used validated subjective questionnaires and physiological measurements to assess the effects of a 50 mg dose of BZP in group of female volunteers. The researchers found that BZP increased heart rate and blood pressure and produced subjective effects similar to other stimulants such as dexamphetamine and MDMA. Participants given BZP experienced decreased fatigue and a lack of appetite, as well as a significant increase in subjective ratings of ‘drug-induced euphoria’ on a scale intended to measure ‘feelings of popularity, efficiency, social effectiveness, pleasant feelings, absence of worry, good self-image and feelings of insight and satisfaction’ (Foltin & Fischman Citation1991). However, the BZP group also displayed an increased score on a scale measuring ‘dysphoria and somatic complaints’ (Foltin & Fischman Citation1991).
A qualitative study of BZP users revealed that despite common adverse effects, most users considered the unwanted side effects tolerable when balanced against the desired effects of increased energy and sociability (Butler & Sheridan Citation2007). Further qualitative research also revealed that the popularity of BZP party pills amongst youth was in part related to their legal status and perceived safety—despite the fact that at the time there had been no modern controlled studies examining the effects on humans (Sheridan & Butler Citation2009).
It should be noted that according to STANZ there has been no record of any death, long-lasting injury or illness attributed solely to BZP (STANZ Citation2008). There have, however, been several deaths in which BZP was a factor in conjunction with other illicit drugs (Balmelli et al. Citation2001; Wikstrom et al. Citation2004; Elliott & Smith Citation2008). Case reports have also noted BZP ingestion producing dissociative states (Wood et al. Citation2008), psychosis (Austin & Monasterio Citation2004), precipitation of mania in schizophrenia (Mohandas & Vecchio Citation2008), and organ failure (Alansari & Hamilton Citation2006; Gee et al. Citation2010).
Legality of BZP in New ZealandBenzylpiperazine was initially marketed during the 1999–2005 period without regulation in New Zealand and was presented initially as a tool for decreasing methamphetamine addiction, which was of growing concern to the public (May Citation2006). Following the unexpected popularity of BZP products, the substance was reviewed by the Expert Advisory Committee on Drugs (EACD), a group of medical and public health experts designated to provide advice to the Ministry of Health.
In 2004, the EACD advised the Associate Health Minister (Hon Jim Anderton) that while there was no direct evidence of serious harm, BZP and its effects were poorly understood. They recommended that the government undertake further research to determine the exact extent and impact of BZP use in New Zealand. They did not advocate legislation criminalizing BZP but suggested that the substance be more carefully regulated, and further research into it effects be carried out (EACD Citation2004). In response to the advice of the EACD, the Associate Health Minister added a supplementary order paper to an amendment bill, providing for a new schedule of controlled substances termed ‘restricted substances’ (referred to as Schedule 4 in the new legislature). ‘Restricted substances’ were still legal to possess and sell, but were subject to an age limit on sales (18 years or older) and there were restrictions on the advertising and locations of sale for such products. The amendment also made provision for controls on dosage and labelling, as well the establishment of a manufacturing code (though specifications for these elements were never made or enforced by the Governor General or Director-General of Health [Dawkins Citation2008]). The bill passed its first reading in September 2004 and was referred to a select health committee and public submissions were considered. In 2005 the bill was read a second and third time before being passed into law by royal assent on 25 June (Misuse of Drugs amendment Act 2005). This was the first such legislation in the developed world to provide a legally available and regulated psychoactive substance of no therapeutic value (discounting the long-standing legality and regulation of alcohol and tobacco).
The following year the EACD examined new evidence, including surveys, human studies, and clinical reports previously referred to (full details of the information considered by the EACD can be found in the publically available reports to the Minister [EACD Citation2006, Citation2007]). Based on the new information the EACD issued a letter of advice to the Associate Health Minister. The committee determined that, based on the available information, BZP posed ‘moderate risk’ and should be reclassified as a Class C1 controlled substance (equivalent to cannabis)—making BZP illegal to sell or possess (EACD Citation2006). The Associate Health Minister put a bill to this effect forward and a formal public consultation process was undertaken. After considering the public submissions as well as several new or updated studies, the EACD reiterated their position a year later in a similar report to the Associate Health Minister (EACD Citation2007). Following several parliamentary debates, an amendment was passed in March 2008, to come into effect on 1 April 2008, re-classifying BZP as a Class C drug. Sale of BZP was immediately prohibited and, after a 6-month amnesty period, possession of BZP became a convictable offence (Misuse of Drugs (Classification of BZP) Amendment Act 2008).
While the initial Misuse of Drugs Act Amendment Act (2005) created a schedule intended to regulate low-risk psychoactive drugs, it has since been shown to conflict directly with the Hazardous Substances and New Organisms Act 1996 (HSNO). A recent Law Commission review has determined that ‘The restricted substances regime can have no content unless regulations are made under HSNO excluding psychoactive substances that might be brought within the restricted substances scheme from the definition of hazardous substance’(NZLC Citation2010:87).
The effects of BZP prohibition in New Zealand and future issuesThere has been some research investigating the effects of the New Zealand government decision to ban BZP. Prior to the ban being finalised, a survey of students revealed that some BZP users (46%) believed they were more likely to increase their consumption of other illegal drugs—particularly ecstasy—following the criminalisation of BZP (Green Citation2008). Another study in a targeted sample of regular BZP users found similar results, with ecstasy again being a common choice of drug in the absence of BZP (Bryson & Wilson Citation2007). These studies agree with preliminary results from a survey of BZP users conducted before and shortly after BZP prohibition came into effect (Sheridan et al. Citation2009): among a minority of drug users, demand for illegal substances increased in the absence of easily accessible and legal BZP. However, the authors noted that the short time frame of their study was a limiting factor and they felt the full impact of the ban may take some time to become apparent. The study also found that the prohibition of BZP had been effective in decreasing BZP consumption. Research from the Massey University Illicit Drug Monitoring System, which gathers data from a sample of frequent drug users, revealed that prohibition of BZP resulted in a substantial decrease in the availability of BZP. Users reported that BZP was more difficult to obtain, supplies were less reliable and the cost had increased considerably (Wilkins et al. Citation2009). Although this indicated that prohibition was effective in decreasing use, the researchers also speculated that the ban may have contributed to an increase in ecstasy use found in their survey (Massey Citation2009).
While BZP retailers were forced to comply with the law and cease selling BZP, many suppliers have grasped the opportunity to cater to consumer's continued demand for ‘party pills’. A variety of new ‘BZP-free’ pills such as the ‘Elements’ range (
www.evolvetech.co.nz) and ‘Go-E’ (
www.cosmiccorner.co.nz) have replaced the now illegal BZP products on the shelves. These pills containing dimethylamylamine (DMAA; often defined as ‘geranium extract’) have been widely marketed in New Zealand since the ban. There have been several hospitalisations due to side effects such as nausea and vomiting—and in one case, stroke following consumption of DMAA (Chalmers Citation2008, Citation2009). There has been recent pressure from politicians to schedule DMAA as a schedule 4 restricted substance, a move welcomed by STANZ, who advocate the regulation of commercial legal highs (Steward Citation2009). Such a scenario does not appear to be possible at this stage, given the legal conflict noted by the Law Commission review.
Summary and conclusionsBenzylpiperazine is a substance that has been under-examined since it was first synthesised over 60 years ago. It has an effect similar to amphetamine in humans and can cause some adverse symptoms. The lack of information regarding BZP and its effects became most apparent when the drug was legally introduced onto the New Zealand market. Following the sudden popularity of BZP party pills, in 2005 the New Zealand government introduced unique legislation to regulate, rather than prohibit, the substance. In light of further research and medical concerns, sale and possession of
BZP was criminalised in 2008. Preliminary research indicates that criminalisation has been effective in decreasing use of BZP although there is some evidence suggesting prohibition may have led to an increase in consumption of other illicit drugs for a minority of pre-ban BZP users. There has also been an increase in the sale of BZP-free party pills, which may contain unregulated substances with dubious safety records.